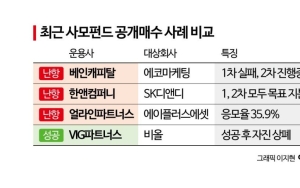
Financial Supervisory Service Discloses Key Cases of Insurance Payment and Non-Payment Reasons
 [Photo by Getty Images Bank]
[Photo by Getty Images Bank]
Recently, office worker Mr. A, who had been suffering from toothache, could no longer endure it and pulled out his loose tooth by himself at home. Afterwards, he visited a dental clinic, received implant treatment, and claimed insurance benefits for prosthetic treatment costs. However, the insurance company denied the payment, citing that Mr. A had extracted the tooth himself without consulting a dentist.
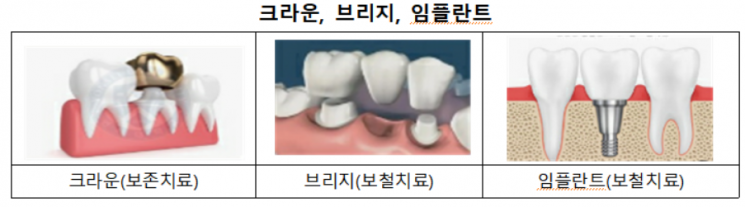
The dental insurance policy stipulates that insurance benefits are paid only when a permanent tooth extraction diagnosis is made by a dentist at a hospital or dental clinic, and prosthetic treatment (such as dentures, bridges, implants, etc.) is performed on the extraction site. It should not be misunderstood that simply having a prosthetic device installed at a hospital guarantees insurance payment.
On the 3rd, the Financial Supervisory Service disclosed major complaint cases related to reasons for insurance payment and non-payment (exemption reasons). This is due to the continuous increase in disputes between policyholders and insurance companies as third-party insurance covering illness, injury, and nursing care becomes more diversified and complex.
Insurance benefits are also not paid when repairing or replacing previously treated prosthetics. The dental insurance policy specifies that insurance benefits are not paid for repairing, restoring, or replacing dental restorations or prosthetics.
Even if one enrolls in insurance and receives treatment while in need of treatment for cavities or periodontitis, insurance benefits may not be paid. The policy clearly states that insurance benefits are paid only if prosthetic or conservative treatment is diagnosed and received after insurance enrollment for cavities or periodontal disease. Prosthetic treatment refers to treatments that replace teeth by creating artificial teeth such as implants or dentures. Conservative treatment refers to treatments that preserve teeth without extraction, such as resin or amalgam fillings.
For bridges and implants, insurance benefits are calculated based on the number of permanent teeth extracted. Even if one extracts one permanent tooth and receives bridge treatment connecting prosthetics to adjacent teeth, insurance benefits are paid only for prosthetic treatment of one tooth.
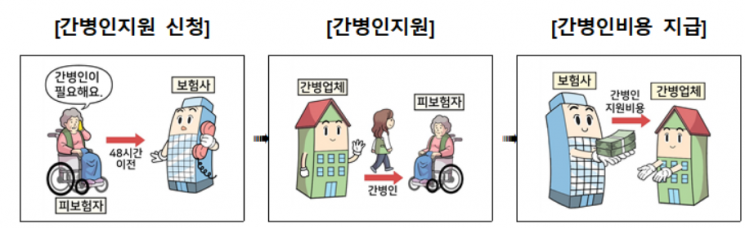
Disputes also persist regarding nursing care, surgery, and hospitalization. Office worker Mr. B recently enrolled in the 'Nursing Care Support Hospital Daily Allowance Rider' and was hospitalized for a spinal disease. Afterward, he arbitrarily used a caregiver and claimed the caregiver expenses as insurance benefits, but only a small daily hospitalization allowance was paid.
The Nursing Care Support Hospital Daily Allowance Rider policy states that to receive caregiver support, one must apply to the insurance company for nursing care support at least 48 hours in advance. If a caregiver is used arbitrarily, only the daily hospitalization allowance is provided. When nursing care support is requested from the insurance company, the insurer provides a caregiver, but if support is inevitably impossible, insurance benefits are paid up to the nursing care support cost limit (130,000 to 170,000 KRW per day). Otherwise, a daily hospitalization allowance (10,000 to 30,000 KRW per day) is paid. To receive insurance benefits after using a caregiver, one must enroll in the 'Caregiver Daily Use Rider.'
Surgical insurance benefits may not be paid if the surgery does not meet the methods specified in the policy. For example, if one undergoes an incision surgery to treat a boil on the face and claims disease surgery insurance benefits, payment may be difficult. This is because the policy defines surgery as procedures involving amputation or excision on the living body. Medical procedures with mild invasiveness, such as simple incisions, are difficult to cover.
Daily hospitalization allowances for injury or illness are recognized only when the hospitalization is directly for treatment of the injury or illness. Office worker Mr. C was hospitalized to treat a rotator cuff tear caused by being caught in a subway door. During hospitalization, he developed indigestion and gastroesophageal reflux disease and received treatment for these illnesses concurrently. Mr. C received injury hospitalization daily allowance from the insurer and then additionally claimed illness hospitalization daily allowance, but the insurance payment was denied. Even if illness treatment is conducted during hospitalization for injury treatment, compensation is difficult if the necessity of hospitalization for illness treatment is not recognized.
© The Asia Business Daily(www.asiae.co.kr). All rights reserved.
![Clutching a Stolen Dior Bag, Saying "I Hate Being Poor but Real"... The Grotesque Con of a "Human Knockoff" [Slate]](https://cwcontent.asiae.co.kr/asiaresize/183/2026021902243444107_1771435474.jpg)















