H1: First Half Actual Loss Insurance Losses Up 21%
Consumer Complaints Increase Due to Stricter Review
"Desperate Measures Are Urgently Needed at This Time"
[Asia Economy Reporter Oh Hyung-gil] Since last September, Jeon Yunsu (38, pseudonym) has been receiving manual therapy for his neck and shoulders at a Korean medicine hospital and has been diligently claiming the hospital bills from his insurance company. This was because he was informed by the insurer before starting treatment that manual therapy would be covered without any limit on the number of sessions.
Jeon received insurance payouts four times in total. However, he recently received a call from an insurance company representative saying, "Since the manual therapy sessions have exceeded 30, we will conduct an on-site inspection." Jeon expressed anxiety, saying, "I was diagnosed with straight neck and just received treatment," and "I’m worried that if I undergo a separate review, I might not receive insurance payments or might not be able to claim in the future."
As cases of claiming manual therapy costs under indemnity health insurance have surged, insurance companies are significantly strengthening related reviews. This is a 'last resort' measure to manage the rapidly increasing loss ratio of indemnity insurance.
Although the stricter reviews have led to growing resistance from policyholders, the stance is that it is unavoidable since a considerable portion of illegal or excessive claims originate from manual therapy.
According to the insurance industry on the 11th, insurance companies plan to strengthen on-site inspections for cases with many manual therapy sessions and tighten underwriting reviews for agents with high musculoskeletal loss ratios starting in the second half of the year.
This is an additional countermeasure following earlier efforts such as raising the eligible age for new indemnity insurance subscriptions, strengthening underwriting reviews to raise the entry barrier, and suspending sales.
An official from a non-life insurance company said, "This is a measure to strengthen the review criteria for manual therapy that is excessively performed to manage appropriate loss ratios. If there is no violation of the duty of disclosure and the treatment was received for medical purposes, there is no problem with insurance payment. However, if the treatment was received for reasons such as correction rather than therapy, insurance payments may be denied."
The More Indemnity Insurance Is Sold, the More 'Losses' Occur
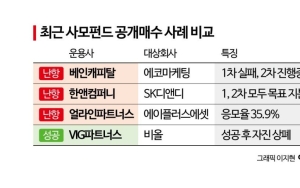
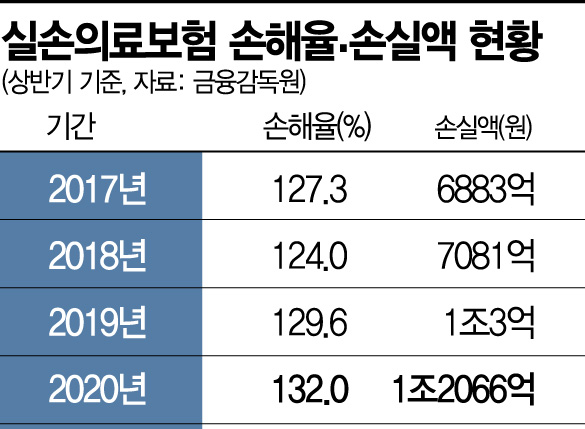
The reason insurance companies have resorted to drastic measures is that the scale of losses from indemnity insurance has reached a serious level this year. Due to the decrease in hospital visits during the first half of the year caused by the novel coronavirus disease (COVID-19), the loss amount for indemnity insurance has increased by 20.6% compared to last year, reaching 1.2066 trillion KRW.
The loss ratio for indemnity insurance stands at 132%, up 2.4 percentage points from the same period last year. Insurance companies have pointed to non-reimbursable items such as manual therapy and nutritional injections as the main culprits behind the rising loss ratio. Unable to withstand the loss ratio, 11 out of 19 insurers that handled indemnity insurance have suspended sales in the first half of this year.
The problem is that some hospitals are still attracting customers by promoting that manual therapy can be received without cost burden if indemnity insurance is used.
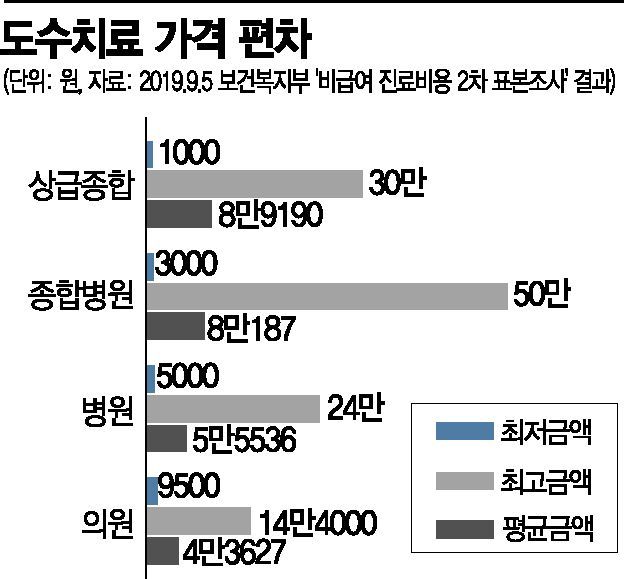
Manual therapy is a non-reimbursable item not covered by the National Health Insurance benefits, so patients must bear the full cost of treatment. However, with indemnity insurance, manual therapy can be received up to 180 times per year. In particular, there are no clear review criteria for manual therapy, and it is promoted that insurance claims can be easily made as long as there is a doctor's diagnosis.
An official from an insurance company selling indemnity insurance pointed out, "If the loss ratio of indemnity insurance soars, it will eventually be reflected in the overall annual loss ratio, resulting in a vicious cycle that leads to premium increases for many policyholders."
Some voices argue for differentiated indemnity insurance premiums, where those who claim more insurance benefits should pay higher premiums. According to the Korea Insurance Research Institute, over 90% of all indemnity insurance subscribers have not claimed insurance benefits, while about 2% claim more than 1 million KRW annually.
© The Asia Business Daily(www.asiae.co.kr). All rights reserved.

![Clutching a Stolen Dior Bag, Saying "I Hate Being Poor but Real"... The Grotesque Con of a "Human Knockoff" [Slate]](https://cwcontent.asiae.co.kr/asiaresize/183/2026021902243444107_1771435474.jpg)















