Insurance Benefits Not Payable for Purely Cosmetic Purposes
Office worker Park Ji-eun (32, pseudonym) usually suffers from severe rhinitis and underwent nasal valve reconstruction surgery (rhinitis surgery) with both nasal congestion treatment and cosmetic effects at a hospital located in Gangnam-gu, Seoul. Park later filed an insurance claim, but the payment was denied because there was no medical record confirming nasal valve stenosis at the hospital.
Nasal valve reconstruction surgery is a procedure to widen the nasal valve to relieve nasal congestion symptoms caused by nasal valve stenosis. It is a new medical technology approved by the Minister of Health and Welfare and is used only for approved purposes and patients. To receive insurance payment, nasal valve stenosis must be confirmed through tests such as 3D-CT scans. If the purpose is solely cosmetic improvement, payment will be denied.
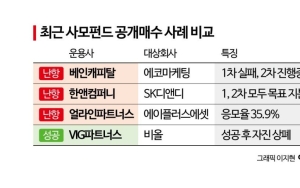
The Financial Supervisory Service disclosed on the 4th common complaint cases frequently occurring in indemnity insurance. Many subscribers mistakenly believe that indemnity insurance reimburses the full amount of medical expenses, so this measure aims to prevent economic losses due to high medical costs.
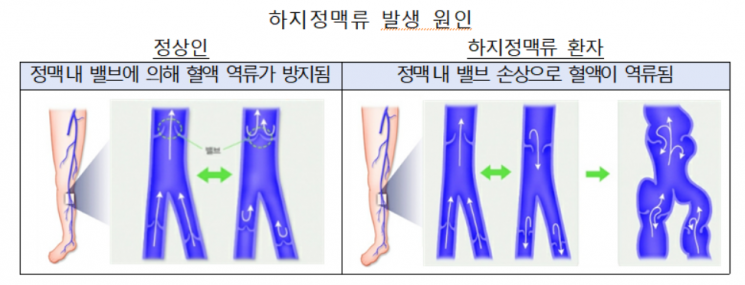
When claiming insurance for varicose vein surgery, medical records that can confirm the diagnosis, such as ultrasound examination records, must be submitted. Varicose veins are a condition where the venous valves in the lower limbs malfunction, causing blood to flow backward and veins under the skin to abnormally enlarge and protrude outside the skin. Typically, varicose veins are diagnosed when blood reflux of more than 0.5 seconds is confirmed through ultrasound examination. If ultrasound examination records are not submitted, the surgery may be judged as cosmetic (removal of veins protruding outside the skin), and insurance payment may be denied.
Double eyelid surgery solely for cosmetic improvement is not covered by insurance. The Ministry of Health and Welfare specifies double eyelid surgery that is not for essential bodily function improvement as a ‘non-reimbursable service.’ If the medical fee for double eyelid surgery is billed as ‘non-reimbursable,’ it is considered cosmetic surgery, and insurance payment will not be made. However, if the Health Insurance Review and Assessment Service’s medical fee confirmation shows that the double eyelid surgery fee has changed from non-reimbursable to reimbursable, the insured can reapply for insurance payment. Double eyelid surgery for disease treatment purposes, such as ptosis (drooping eyelid) or entropion (eyelid turning inward causing eyelashes to irritate the eye), is also covered.
Even if for disease treatment, costs for purchasing glasses, contact lenses, crutches, hearing aids, or orthoses are not covered. However, exceptions apply when artificial organs are implanted in the body to replace their function. Additionally, costs unrelated directly to disease treatment, such as preventive health checkups, vaccination fees, and issuance of medical certificates, are not covered.
© The Asia Business Daily(www.asiae.co.kr). All rights reserved.
![Clutching a Stolen Dior Bag, Saying "I Hate Being Poor but Real"... The Grotesque Con of a "Human Knockoff" [Slate]](https://cwcontent.asiae.co.kr/asiaresize/183/2026021902243444107_1771435474.jpg)















