[Asia Economy Reporter Changhwan Lee] A large number of people who were deceived by insurance fraud brokers linked to a Korean medicine clinic in Seoul and prescribed Gongjindan, which is not covered by indemnity insurance, and received indemnity insurance payments have been caught.
On the 17th, the Financial Supervisory Service (FSS) warned that illegal brokers who lure patients with indemnity insurance are conspiring with hospitals to defraud insurance money from patients, and this insurance fraud method is widespread.
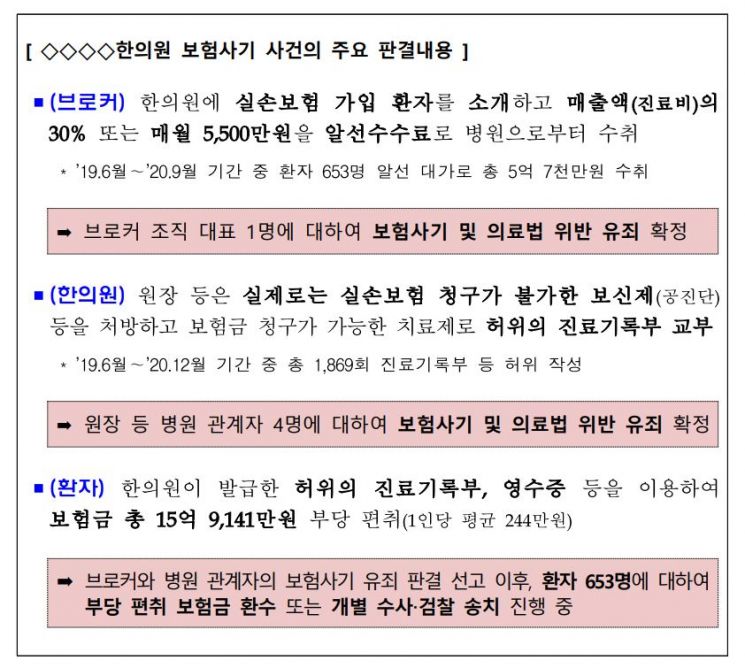
According to the FSS, a recent guilty verdict was confirmed in a case where 653 patients who fraudulently obtained insurance money using false receipts issued by a Korean medicine clinic introduced by an insurance fraud broker were caught as accomplices in insurance fraud.
They were found to have visited a Korean medicine clinic in Seoul introduced by a broker who advertised, "We will process so that you can purchase Gongjindan, which cannot be claimed under indemnity insurance, with insurance money," received prescriptions for Gongjindan, and falsely received indemnity insurance payments.
The broker introduced patients with indemnity insurance to the Korean medicine clinic and received brokerage fees of 30% of sales (treatment fees) or 55 million KRW per month from the hospital.
The clinic director and others prescribed Boshinje (Gongjindan), which is actually not claimable under indemnity insurance, and issued false medical records indicating treatments eligible for insurance claims. Four hospital officials, including the director, were convicted of insurance fraud and violations of the Medical Service Act.
The patients fraudulently obtained a total of 1,591,410,000 KRW (an average of 2,440,000 KRW per person) in insurance money using false medical records and receipts issued by the Korean medicine clinic.
An FSS official emphasized, "Claiming insurance money using certificates and receipts that were falsely prepared constitutes insurance fraud," and urged, "Please be cautious not to be involved in illegal activities by being enticed by hospitals or brokers offering to process insurance for treatments not covered by insurance."
The FSS requested active reporting to the 'Insurance Fraud Reporting Center' if anyone receives insurance fraud proposals from hospitals or brokers or becomes aware of suspicious cases.
If the report is confirmed as insurance fraud, the Insurance Association or insurance companies will pay rewards up to 1 billion KRW according to the reward payment standards.
© The Asia Business Daily(www.asiae.co.kr). All rights reserved.
![Clutching a Stolen Dior Bag, Saying "I Hate Being Poor but Real"... The Grotesque Con of a "Human Knockoff" [Slate]](https://cwcontent.asiae.co.kr/asiaresize/183/2026021902243444107_1771435474.jpg)















