Conflict Between Medical and Insurance Industries Over Intermediary Institutions
Prioritizing Public Convenience... Utilizing Platforms
Insurance Business Act Passed by National Assembly After One Year of Discussions
The Presidential Commission on the Digital Platform Government (DPLG) was launched on September 1 last year. One of DPLG's important roles was to provide digital services that the public wants in a simple and easy way. What digital service did the public want the most? According to a public survey conducted earlier by the Presidential Transition Committee, "simplification of claims for indemnity health insurance" received the highest vote rate and was selected as number one. Simplifying indemnity insurance claims has also been a long-standing wish of the insurance industry for 14 years. Therefore, DPLG rolled up its sleeves. About 20 stakeholders from the medical and insurance industries, related government departments, and consumer groups held more than 10 meetings over about a year to resolve this long-standing issue.
We heard the behind-the-scenes story through an interview with Professor Kim Hyung-sook of Hanyang University (Director of Hanyang Digital Healthcare Center), who led the simplification of indemnity insurance claims in the health and medical leading task force (TF) under DPLG.
Medical and Insurance Industries Clash Over Intermediary Institution for 14 Years
Until now, indemnity insurance subscribers had to submit documents such as receipts received from hospitals directly to insurance companies via fax or applications. Everyone has probably experienced inconvenience during the insurance claim process at least once. From the hospital's request to "wait a few days for the doctor's signature on the documents" to the insurance company's demand for "additional documents," these inconveniences have been common. Due to these inconveniences, a survey found that the annual unclaimed indemnity insurance amount reaches 276 billion KRW. For the past 14 years, related organizations have failed to reach an agreement and have been in sharp conflict, causing mental and financial damage to the public. Professor Kim said, "For 14 years, they only argued their own points," adding, "We had to differentiate the way to solve the problem from the existing methods."
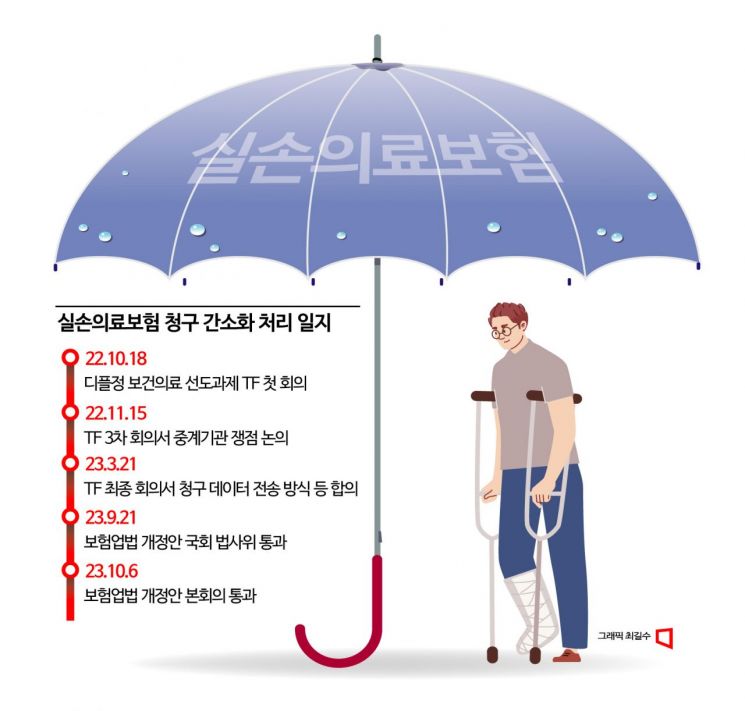
On October 18 last year, Professor Kim gathered representatives from the medical community, insurance industry, Ministry of Health and Welfare, and Financial Services Commission to hold the first TF meeting. Interestingly, all parties agreed on the direction of promoting simplified indemnity insurance claims. The problem was who would be the 'intermediary institution' that provides the subscriber's indemnity insurance claim data from hospitals to insurance companies. The medical community (Korean Medical Association, Korean Hospital Association) had opposed the Health Insurance Review & Assessment Service (HIRA) acting as the intermediary institution, fearing that the government (HIRA) would closely scrutinize non-reimbursable medical records. On the other hand, the insurance industry (General Insurance Association of Korea) insisted that HIRA should be designated as the intermediary institution. The insurance industry believed that since about 10,000 medical institutions open and close annually, a stable public institution like HIRA is more suitable than private entities to serve as the intermediary.
More Than 10 Meetings and Final Discussions
Professor Kim listened to both sides' opinions evenly and held final discussions on △ designating HIRA as the intermediary institution, △ designating a third party as the intermediary institution, and △ proceeding without designating an intermediary institution. He resolved each issue raised by both sides one by one. In this process, public convenience was prioritized, and the means of a 'digital platform' was utilized.
Professor Kim said, "We focused most on achieving the goal that money (insurance benefits) should be quickly deposited into the subscriber's account," adding, "We made it clear that data flows at the speed of light through platform technology and that personal information is not identifiable." They reviewed overseas cases related to indemnity insurance claims in countries such as the UK and France and also searched for domestic fintech companies that could assist the intermediary institution. By persistently engaging in a total of 15 meetings with the medical and insurance industries individually, they were able to reach an agreement on simplifying indemnity insurance claims.
 Professor Hyung-sook Kim, Department of Data Science, Hanyang University, and Director of Hanyang Digital Healthcare Center
Professor Hyung-sook Kim, Department of Data Science, Hanyang University, and Director of Hanyang Digital Healthcare Center
The DPLG agreement includes the following. First, the term 'intermediary institution' was changed to 'transmission agency.' Also, one of the public institutions performing public functions was selected as the transmission agency. This was a key issue that had not been agreed upon for 14 years. Medical record data such as receipts and detailed medical expense statements are encrypted electronically during transmission and are not stored internally. Through consultations between the medical and insurance industries, a dedicated organization for managing and supervising the transmission agency was established, and patients can select their medical details themselves to make claims.
Saving Hundreds of Billions of KRW Through Digital Platform
These efforts by DPLG were carried out quietly behind the scenes. Unlike the previous government, there was no loud slogan of 'social grand compromise.' In particular, the simplification of indemnity insurance claims became a representative case discovering the potential of the platform. The National Assembly took over the baton. Six insurance business law amendment bills proposed by both ruling and opposition parties were integrated and reviewed, incorporating the DPLG agreement. The amended bill sequentially passed the National Assembly's Legislation and Judiciary Committee last month and the plenary session on the 6th.
In the next one to two years, data will be linked and opened between medical institutions and insurance companies, allowing subscribers to conveniently apply for insurance benefits without preparing documents. When an indemnity insurance subscriber expresses the intention to claim insurance benefits at a hospital, the hospital will send the related documents to the insurance company through the transmission agency. Once the amended insurance business law is enforced, it is expected to simplify more than 50 million claims annually and benefit at least 10 million people. It is also anticipated to save a total of 250 billion KRW, including costs for issuing supporting documents and hospital visits. DPLG stated that by utilizing a digital platform applying private technology, about 10 billion KRW in budget for newly building the indemnity insurance claim electronic network can be saved.
© The Asia Business Daily(www.asiae.co.kr). All rights reserved.