99.7% Procedural Success Rate
Atrial septal defect is a congenital heart disease in which there is a hole in the wall between the right and left atria, causing blood to leak into the right atrium. It is often treated with a procedure that inserts a closure device through a catheter to seal the hole between the atria. In this procedure, it is important to select a closure device that precisely matches the size of the atrial hole, but there had been no standardized international guidelines for choosing the size of the closure device.
According to Asan Medical Center on February 26, a cardiology team led by Professor Song Jongmin recently announced research findings showing that, when they used three-dimensional echocardiography before percutaneous closure of an atrial septal defect to precisely measure the size and shape of the atrial hole and then selected the closure device accordingly, the procedural success rate reached 99.7%, greatly improving safety and efficiency.
 Professor Song Jongmin, Department of Cardiology, Seoul Asan Medical Center. Seoul Asan Medical Center
Professor Song Jongmin, Department of Cardiology, Seoul Asan Medical Center. Seoul Asan Medical Center
As this is the largest study to date validating the outcomes of percutaneous closure of atrial septal defects using three-dimensional echocardiography, it is expected to contribute to establishing guidelines for determining the size of closure devices.
Atrial septal defects are usually asymptomatic, so they are often diagnosed either through screening in newborns or after symptoms develop in adulthood. As blood leaks into the right atrium through the atrial hole, patients may experience fatigue or shortness of breath, and in severe cases it can progress to serious complications such as heart failure, pulmonary hypertension, arrhythmia, and stroke, making treatment necessary.
Recently, instead of open-heart surgery, percutaneous closure has become the main treatment method. In this procedure, a catheter is inserted through a leg vein and a closure device is fixed in the hole between the atria to close the defect.
If the closure device is too small relative to the atrial hole, there is a risk that the device will not remain fixed and may dislodge. If it is too large, it can continuously irritate and damage the surrounding tissue. Therefore, determining the appropriate size of the closure device is extremely important.
To determine the size of the closure device, the conventional approach has mainly relied on the balloon sizing method, in which a balloon is inserted into the defect area during the procedure, inflated, and its diameter measured. This method can overstretch the atrial septum, increasing the likelihood of selecting a device larger than actually needed, and if the measurement time is prolonged, it can, in rare cases, lead to complications such as cardiac injury.
To address this, three-dimensional transesophageal echocardiography, which involves inserting an ultrasound-equipped endoscope into the esophagus to visualize the heart in 3D, has recently come into use. It allows clear visualization of the internal cardiac structures from multiple angles.
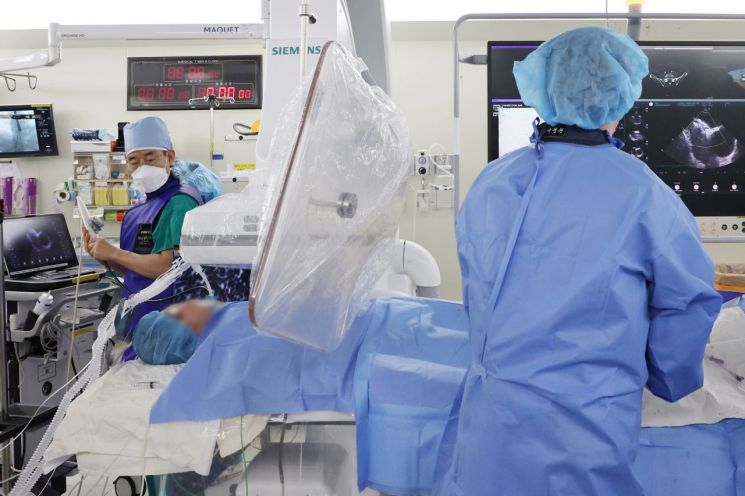 Song Jongmin, Professor of Cardiology at Asan Medical Center (left), is performing percutaneous closure of an atrial septal defect while precisely identifying the defect with echocardiography during the procedure. Prior to the procedure, three-dimensional transesophageal echocardiography was performed to accurately measure the size and shape of the atrial defect, greatly improving procedural success and safety. Asan Medical Center
Song Jongmin, Professor of Cardiology at Asan Medical Center (left), is performing percutaneous closure of an atrial septal defect while precisely identifying the defect with echocardiography during the procedure. Prior to the procedure, three-dimensional transesophageal echocardiography was performed to accurately measure the size and shape of the atrial defect, greatly improving procedural success and safety. Asan Medical Center
The team led by Professor Song Jongmin followed 748 adult patients with atrial septal defects who underwent percutaneous closure at Asan Medical Center between September 2016 and May 2024. For these patients, the size of the closure device was predetermined using three-dimensional transesophageal echocardiography before the procedure. The outcomes were tracked for an average of 1.6 years. As a result, the procedural success rate was 99.7%, and there were no deaths attributable to cardiac causes during the follow-up period.
Of the 748 cases, excluding 2 failures due to device malfunction, there was only 1 case in which the closure device had to be resized during the procedure. Only 1 case required conversion to surgery. It was interpreted that by accurately measuring the maximum and minimum diameters of the atrial hole before the procedure using 3D echocardiographic imaging, the need for repeat procedures and procedural errors was greatly reduced.
In addition, by pre-determining the device size using 3D echocardiographic imaging, the procedure time was also significantly shortened. The average procedure time was 18 minutes, more than halving the 45 to 66 minutes typically required when using the traditional balloon sizing method.
Professor Song Jongmin of the Cardiology Department at Asan Medical Center said, "By accurately assessing the size and shape of an atrial septal defect with three-dimensional transesophageal echocardiography before the procedure, we can reduce the risk of complications that may occur during balloon sizing, and also decrease both the procedure time and radiation exposure. Through this study, we also found that about 25% of patients have oval-shaped atrial septal defects and that the longest axis of the defect varies greatly from patient to patient. When using the conventional balloon sizing method, there is a risk that the size of the hole will be underestimated by up to 35%. Taking this into account, determining the size of the closure device using three-dimensional transesophageal echocardiography may be the best approach."
The study results were recently published in the European Heart Journal - Cardiovascular Imaging, a leading international journal (impact factor 6.6).
Meanwhile, Asan Medical Center treats 1 out of every 5 adult atrial septal defect patients in Korea, leading the field of cardiac care. The hospital is actively applying in clinical practice the use of three-dimensional transesophageal echocardiography to determine the size of closure devices instead of the balloon sizing method. It also uses three-dimensional echocardiography to pre-screen defect morphologies that are not suitable for percutaneous closure, thereby avoiding unnecessary procedures, providing optimal treatment, and improving patients' quality of life.
© The Asia Business Daily(www.asiae.co.kr). All rights reserved.